Introduction to Flat Feet: Understanding Pes Planus
Flat feet, medically referred to as pes planus, is a foot condition where the arches, typically curved, fully touch the ground when a person stands. This lack of arch can significantly influence stability and balance, impacting daily activities and overall mobility. This detailed exploration aims to shed light on the various manifestations of flat feet, investigate their root causes, identify common symptoms, review diagnostic procedures, and present comprehensive management strategies.

Diverse Manifestations of Flat Feet
The Commonality of Flexible Flat Feet
Flexible flat feet stand out as the most common variant, particularly noticeable in children. This condition is characterized by an arch that appears normal when the foot is not bearing weight but flattens once standing or walking commences. Generally, flexible flat feet are associated with little to no discomfort, making this condition a relatively benign variation that often does not hinder the developmental stages of childhood.
The Challenge of Rigid Flat Feet
Rigid flat feet present a stark contrast to their flexible counterparts, as the arch remains flat regardless of weight-bearing status. This condition can cause considerable pain and difficulty in performing activities such as walking or running. The lack of arch flexibility and the pronounced symptoms often necessitate medical intervention to alleviate discomfort and improve mobility.
The Progression of Acquired Flat Feet
Acquired flat feet, or adult-acquired flatfoot deformity, describe the gradual loss of the arch over time. This condition frequently demands medical attention due to its progressive deterioration, which can be influenced by aging, injuries, or underlying health issues. The evolving nature of acquired flat feet highlights the importance of early detection and intervention.
The Genetic Aspect of Congenital Flat Feet
Congenital flat feet are identified at birth and are often passed down through generations, pointing to a genetic predisposition. Initially, this condition may not lead to discomfort or mobility challenges. However, the potential for future issues necessitates vigilant monitoring and, if needed, early intervention to address any discomfort or functional limitations that may arise as the individual grows.
Unraveling the Causes of Flat Feet
The development of flat feet is influenced by a multifaceted array of factors, ranging from genetic predispositions to various health conditions and lifestyle factors. Understanding these underlying causes is pivotal for identifying risk factors and implementing preventive measures.
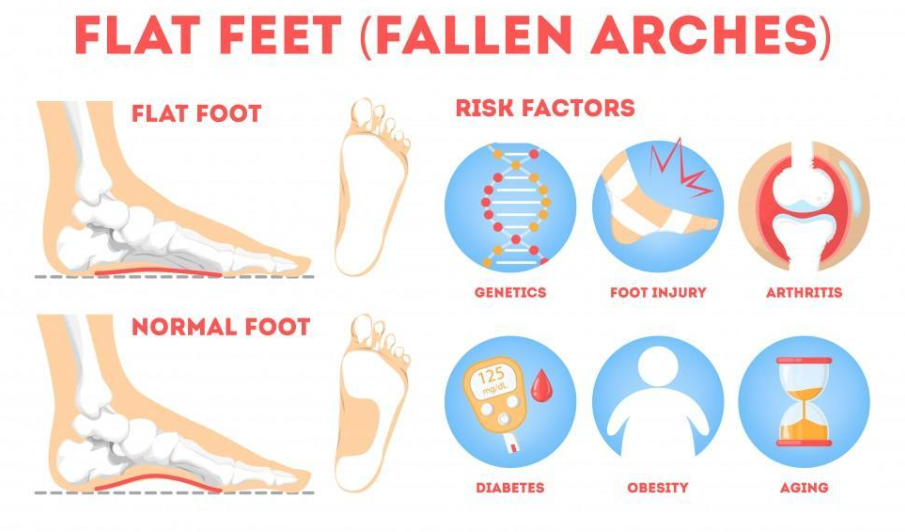
Genetic Factors
A significant contributor to flat feet is genetics. Individuals with a family history of flat feet are more likely to inherit this condition, suggesting a strong genetic component that affects the structural formation of the foot's arch.
Health Conditions
Several medical conditions are known to predispose individuals to flat feet, including:
- Rheumatoid Arthritis: This autoimmune condition can lead to joint inflammation, affecting the foot's structural integrity and potentially flattening the arch.
- Diabetes: Poorly managed diabetes can result in nerve damage and circulatory issues in the feet, weakening the arch over time.
- Obesity: Carrying excess body weight significantly increases the stress on the foot arches, contributing to their eventual collapse.
- Cerebral Palsy: This neurological condition affects muscle tone and coordination, which can alter foot structure and lead to flat feet.
- Muscular Dystrophy: Characterized by progressive muscle weakness, this condition can affect the muscles supporting the foot arch, leading to flat feet.
Lifestyle and Environmental Factors
- Injuries and Overuse: Trauma to the foot, such as fractures or tendon damage, as well as repetitive stress from activities like prolonged standing or intense physical exercise, can lead to the development of flat feet.
- Pregnancy: Hormonal changes during pregnancy, especially the release of relaxin, can loosen ligaments, including those in the feet, leading to temporary or permanent changes in foot structure.
- Aging: The natural aging process can weaken the tendons and ligaments supporting the foot arch, leading to a gradual flattening over time.
Symptoms: The Telltale Signs of Flat Feet
The presence of flat feet can manifest through a variety of symptoms, impacting daily life and overall mobility. Key symptoms include:
- Arch Pain and Discomfort: A common complaint, often exacerbated by prolonged periods of standing or walking.
- Fatigue and Swelling: The feet may tire easily and exhibit swelling, particularly around the ankles and the inner foot area.
- Balance and Posture Issues: The altered foot structure can affect the body's overall alignment, leading to balance difficulties and poor posture.
- Overpronation-Related Symptoms: Excessive inward rolling of the foot can cause heel pain, plantar fasciitis, Achilles tendonitis, shin splints, and knee pain.
- Limited Mobility: Individuals may find it challenging to engage in high-impact activities or wear standard footwear comfortably.
Diagnosing Flat Feet: A Comprehensive Approach
Accurate diagnosis of flat feet is essential for effective treatment and involves a combination of physical assessments and advanced imaging techniques.
Physical Examination
A thorough physical examination by a healthcare professional can assess the foot's structure, range of motion, and muscle strength. Visible signs of arch collapse, especially when bearing weight, are key indicators.
Gait Analysis
Specialized equipment may be used to analyze walking or running patterns, identifying abnormalities such as overpronation that are common in flat feet.
Imaging Tests
- X-rays provide detailed images of the bones, helping to identify structural changes in the arch.
- MRI scans offer insights into the condition of soft tissues, muscles, tendons, and ligaments, useful for diagnosing related conditions.
- CT Scans give a comprehensive view of the foot's internal structure, aiding in the identification of complex abnormalities.
Foot Pressure Mapping
This diagnostic tool measures weight distribution across the soles, highlighting imbalances and guiding the selection of treatment options, such as orthotic inserts or corrective footwear.




